Fatty liver is a metabolic disease, not an alcohol problem, doctors warn
Fri 16 Jan 2026, 02:43:42

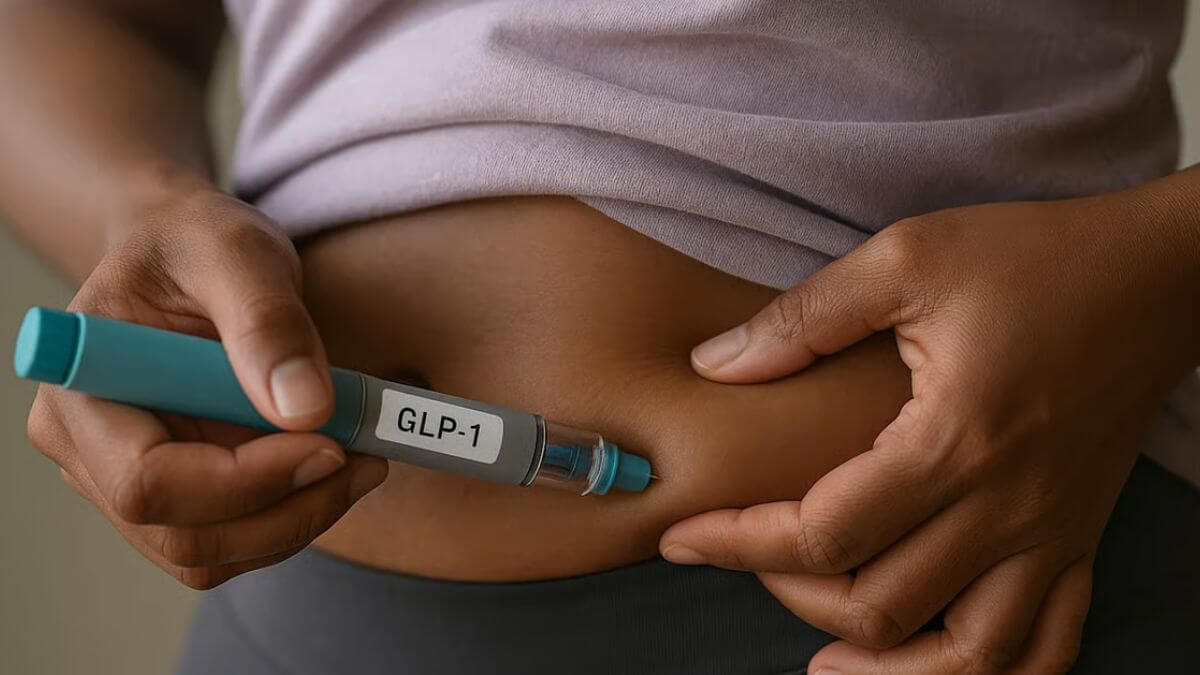
In a recent post on X, hepatologist Dr. Cyriac Abby Philips, popularly known as TheLiverDoc, highlighted a critical but widely misunderstood fact: the most common chronic liver disease worldwide is not caused by alcohol but by non-alcohol–related fatty liver disease, now officially termed Metabolic Dysfunction Associated Steatotic Liver Disease (MASLD).
. The scale of the problem is alarming:
. 30–40% of the general adult population
. 60–70% of people with type 2 diabetes
. 70–80% of individuals with obesity
Despite these staggering numbers, MASLD often remains undiagnosed and untreated, largely because many people assume liver disease only affects those who consume alcohol.
WHAT IS MASLD AND WHY NON-DRINKERS ARE AT RISK
Explaining why teetotallers are increasingly being diagnosed with fatty liver, Dr Daksh Sethi, Bariatric and Laparoscopic Surgeon at Sir Ganga Ram Hospital, Delhi, says MASLD is the liver’s response to metabolic dysfunction.
“Many patients are shocked because they don’t drink alcohol at all,” says Dr Sethi. “MASLD is essentially the liver manifestation of metabolic syndrome.”
In Indians, the risk is amplified by the ‘thin-fat’ phenotype, where individuals may appear lean but carry excess visceral fat around vital organs. Diets high in refined carbohydrates such as white rice, maida, and sugary beverages, combined with sedentary lifestyles, lead to insulin resistance. When the body cannot process glucose efficiently, the liver converts excess sugar into fat, which accumulates in liver cells and triggers inflammation damage that closely resembles alcohol-induced liver injury.
EARLY SYMPTOMS: WHY MASLD IS OFTEN MISSED
MASLD is often referred to as a silent or stealth disease.
“In the early stages, there are almost no clear symptoms,” Dr Sethi explains.
Some individuals may experience:
. Persistent fatigue
. A vague feeling of heaviness
. Mild discomfort or pain in the upper right abdomen
These symptoms are frequently dismissed as gas, acidity, or routine tiredness. Liver blood tests may remain normal until significant damage has already occurred. As a result, MASLD is often discovered incidentally during ultrasounds performed for unrelated conditions such as gallstones.
WHAT HAPPENS IF MASLD IS LEFT UNTREATED
Ignoring fatty liver can have serious and irreversible consequences.
“If untreated, simple fat accumulation can progress to MASH, where inflammation and liver cell injury begin,” says Dr Sethi.
Over time, this progression can lead to:
. Fibrosis (scar tissue formation)
. Cirrhosis, which is irreversible and life-threatening
. Liver failure,
sometimes requiring transplantation
sometimes requiring transplantation
. Hepatocellular carcinoma (liver cancer)
Importantly, MASLD is also a major cardiovascular risk marker. People with untreated MASLD face a significantly higher risk of heart attacks and strokes, which remain the leading cause of death in this population.
WHAT DOES SCIENCE SAY
Medical evidence strongly supports the warnings issued by TheLiverDoc and clinicians on the ground.
A recent review published in JAMA titled “Metabolic Dysfunction–Associated Steatotic Liver Disease in Adults” identifies MASLD as the most common chronic liver disease globally, surpassing alcohol-related liver disease. The review confirms that MASLD is driven by insulin resistance, visceral fat accumulation, obesity, and type 2 diabetes, rather than alcohol intake.
The study shows that MASLD can progress from simple fatty liver to MASH, fibrosis, cirrhosis, liver failure, and liver cancer if lifestyle changes are delayed. Crucially, it concludes that weight loss, dietary modification, and regular physical activity are the most effective and evidence-based treatments, while liver supplements, detox therapies, and pills offer no proven long-term benefit.
The review also highlights that cardiovascular disease not liver failure is the leading cause of death in MASLD patients, reinforcing the need for early metabolic control.
WHAT ACTUALLY WORKS IN TREATMENT
Echoing both the JAMA findings and Dr Cyriac Abby Philips’ message, Dr Sethi stresses that there are no shortcuts.
DIET AND LIFESTYLE ARE THE CORNERSTONE
. Gradual and sustained weight loss
. Avoiding even modest alcohol intake
. Tight control of blood sugar, blood pressure, and cholesterol
FOODS TO LIMIT
. Ultra-processed and processed foods
. Refined sugars, especially fructose
. Saturated fats such as butter, ghee, coconut oil, and lard
EXERCISE PRESCRIPTION
. At least 150 minutes per week of moderate-intensity aerobic activity, or
. 75–150 minutes per week of vigorous exercise
THE SURPRISING ROLE OF COFFEE
Evidence shows that up to three cups of unsweetened black coffee daily may reduce disease progression and liver cancer risk. This recommendation is also included in European liver disease guidelines.
MASLD is common, silent, and dangerous but reversible when caught early.
As Dr Cyriac Abby Philips (TheLiverDoc) has repeatedly warned, detox cures and liver supplements do not fix fatty liver—diet, exercise, and metabolic control do.
And as Dr Daksh Sethi puts it plainly:
“If your doctor isn’t prescribing lifestyle change for MASLD, it’s time to rethink that advice.”
No Comments For This Post, Be first to write a Comment.
Most viewed from Health
AIMIM News
Latest Urdu News
Most Viewed
May 26, 2020
Which cricket teams will reach the IPL 2026 finals?
Latest Videos View All
Like Us
Home
About Us
Advertise With Us
All Polls
Epaper Archives
Privacy Policy
Contact Us
Download Etemaad App
© 2026 Etemaad Daily News, All Rights Reserved.





.jpg)















.jpg)
.jpg)
.jpg)


